Medical Simulation in the Palm of Your Hand
Full Code is an intuitive, mobile-first medical simulation designed by medical practitioners for medical practitioners. With over 170+ medical simulations, realistic-looking virtual patients, and an engaging, gamelike interface, our award-winning app is preferred by medical professionals worldwide.
Full Code Medical Simulation for
Medical Simulation in the Palm of Your Hand
With over 170 medical simulations, realistic-looking virtual patients, and an engaging, gamelike interface, our award-winning app is preferred by medical professionals worldwide.
The #1 Medical Simulation App on the App Store
On-Demand, Virtual Medical Simulation for
Featured Partners and Clients








VP for Interprofessional Education and SimulationRosalind Franklin University
Medical Student Co-clerkship DirectorUniversity of Miami
Miller School of Medicine
Assistant Director of Clinical EducationBoston University Physician Assistant Program
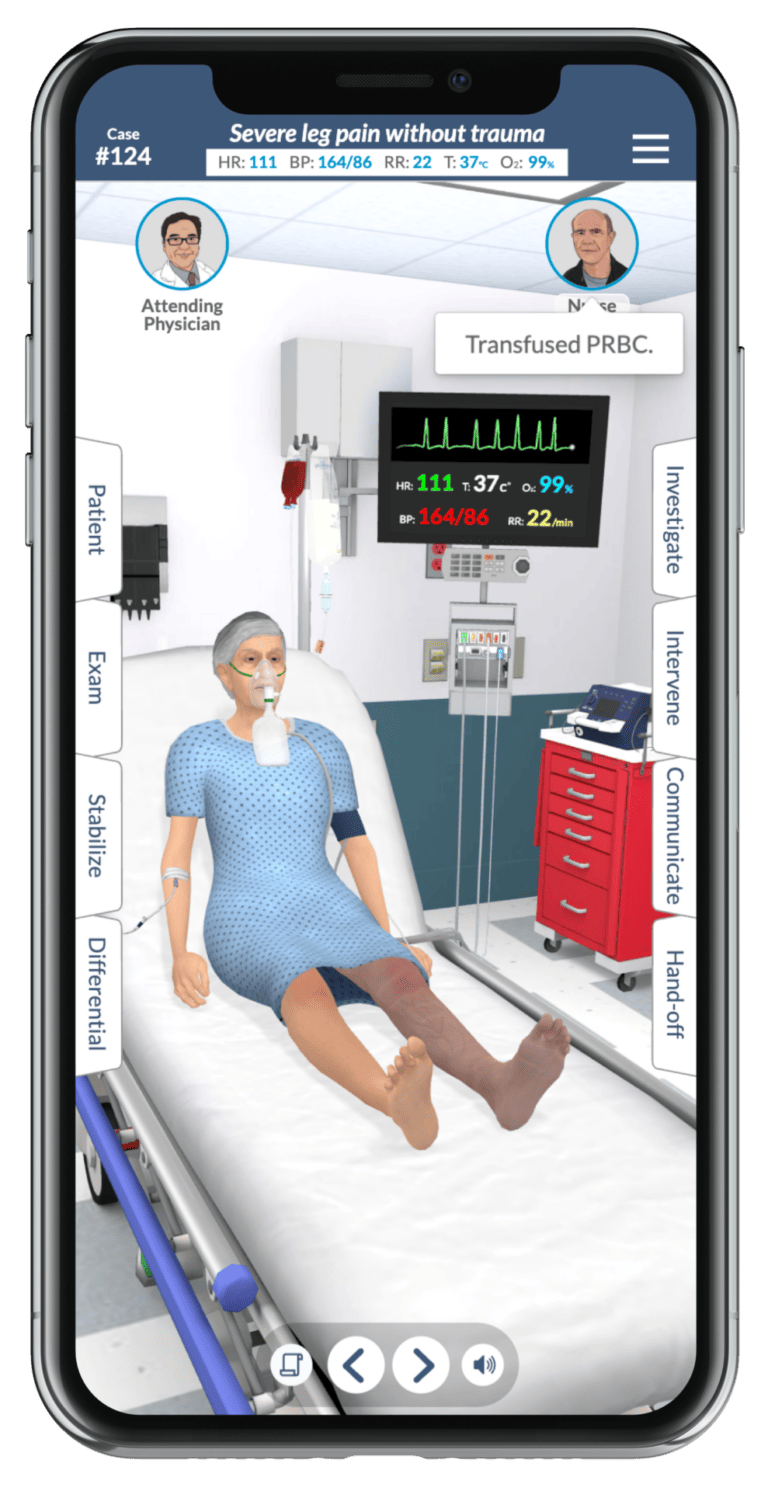
Full Code Features
Medical Simulation Practice Anywhere, Anytime
With traditional simulation training, it can be difficult for students and practitioners to get enough hands-on practice to feel confident on the floor. But at Full Code, we believe that practice makes the practitioner. Improve your skills and save more lives with Full Code Medical Simulation.
Using our immersive virtual simulation platform, medical professionals can practice bite-sized, 3-D medical simulations whenever they get a break, wherever they happen to be. Optimized for portability and accessibility, Full Code is available on any mobile, desktop, or tablet device.
- 170+ cases written by medical professionals
- 31+ specializations
- 4 realistic, immersive 3D environments
- 23 diverse patient avatars, including pediatric and adult patients
- Engaging, interactive simulation design leveraging game theory
- Full score and debrief for each case
- Infinitely repeatable simulations enabling deliberate practice
- Created by medical professionals, for medical professionals.
Want to earn CME credit with Full Code?
How Full Code Can Help
Practice Medical Simulation on the Go
On-demand simulation training with realistic virtual patients allows busy students and medical professionals to practice complex cases and improve their clinical skills anytime, anywhere on the devices they already own.
Easily Identify Knowledge Gaps in Real Time
Our detailed debriefs help learners to identify knowledge gaps and strengthen their skills in weaker areas, helping them to become the best medical practitioners they can be with repeated, hands-on practice.
Improve Confidence and Competence
Full Code's infinitely repeatable cases measure skills in both diagnosis and management, allowing students and medical professionals to learn from their mistakes in a risk-free environment, so they can face complex real world cases without fear.
Level Up with Lessons from the Best
Created by medical educators from some of the top hospitals in the US and peer-reviewed by licensed medical professionals, our simulations are designed in accordance with industry-standard medical best practices, setting the bar high for our learners worldwide.
Save Time and Money
With interactive cases that can be completed anywhere, anytime on any device, Full Code enables you to practice more simulations more frequently using the device you already own, without the time and hassle of scheduling in-person simulation trainings.
Get Started, No Instructions Required
With an intuitive, mobile-first design, Full Code can be used without a complicated instruction manual on a device you already own. Just visit the App Store or Google Play and download the app, or open in a web browser right now to get started.
Interested in purchasing Full Code for your hospital or medical education program?
Full Code Dashboard
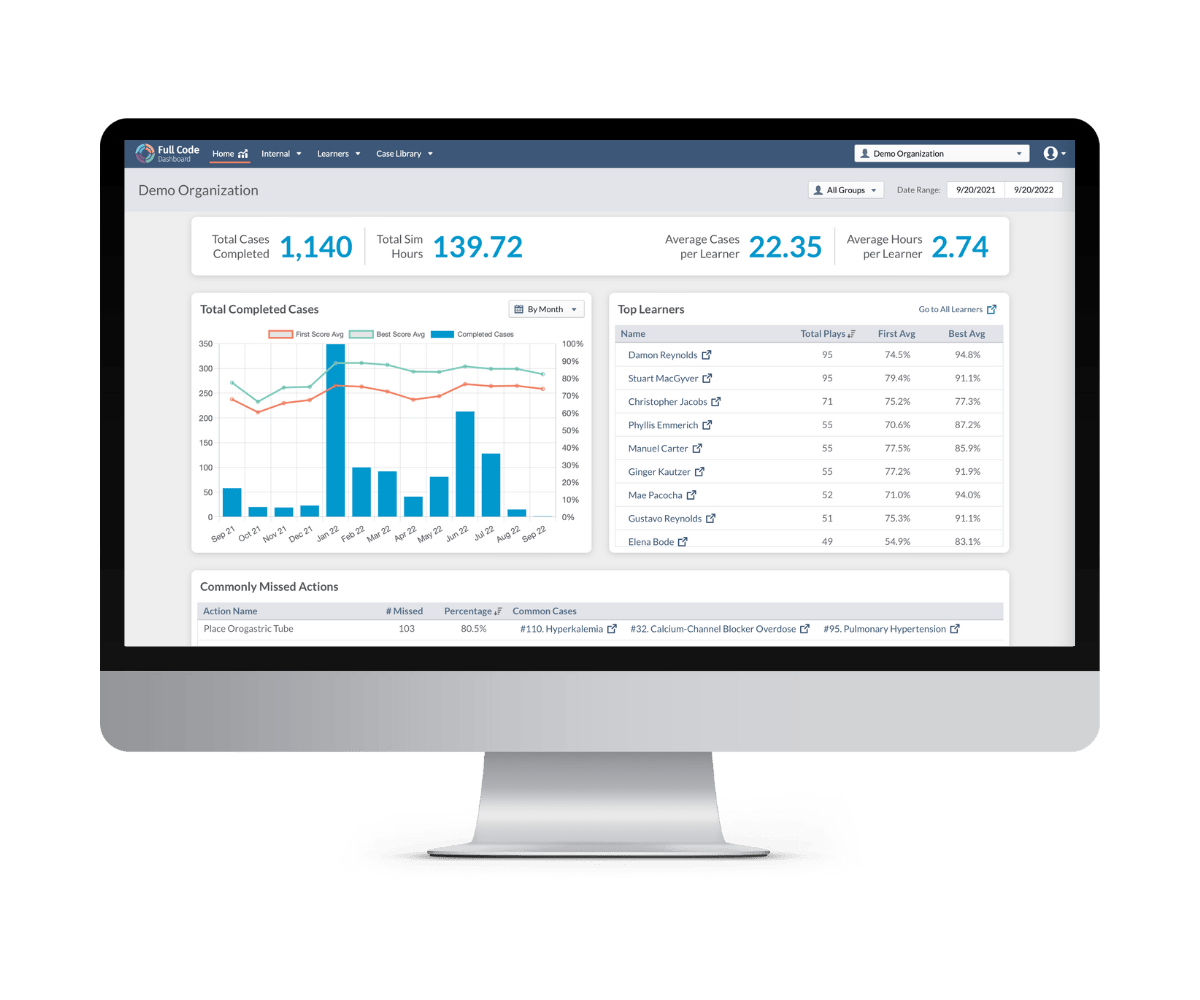
Comprehensive Data for Educators and Administrators
Assess the knowledge of your learners in key areas with the Full Code Dashboard. Full Code records every action learners perform on each case, identifying commonly missed diagnoses, tests, and procedures so that you can analyze their progress every step of the way.
When you log into Full Code Dashboard, you will see a detailed log and summary of every case completed by your learners, tracing their process and identifying areas that need improvement. Aligned with standard medical education practices, Full Code Dashboard enables you to quickly verify that learners have completed requirements and met minimum standards.
Great application for nurses and doctors. It can help you a lot especially when it comes to critical thinking. I hope there are unlimited cases to play. Keep it up.
Alan, Registered Nurse
The Full Code Difference
What makes Full Code different from traditional medical simulation, or other virtual simulation solutions? Find out how you can save time and improve outcomes with Full Code.
Designed for Competency
Full Code offers learners a safe environment for experiential learning. So when the time comes to save real patients, practitioners are ready to tackle complex problems without fear.
Created by Top Clinicians for Clinicians
With a combined 50+ years in the medical field, our expert clinical team leverages their hands-on experience to make each virtual simulation as accurate as possible.
Customizable for Your Unique Needs
Fully customize any of our 170+ pre-existing cases, or design your own. With our signature Full Code Creator tool, instructors are able to bring their own case simulations to life.
Accredited for CME
To offer even more value to medical professionals, we have partnered with Oakstone Publishing to provide AMA PRA Category 1 Credits™ for the successful completion of Full Code cases.
Preferred by Medical Professionals
With over 1 million downloads and a 4.8-star App Store rating, the award-winning Full Code software is the preferred simulation app for medical students and practitioners worldwide.
Optimized for Accessibility
Our mobile-first software is available anywhere, anytime on any device. Intuitive and engaging, it minimizes the learning curve and enables accessibility for all technology comfort levels.
Experience the Full Code Difference
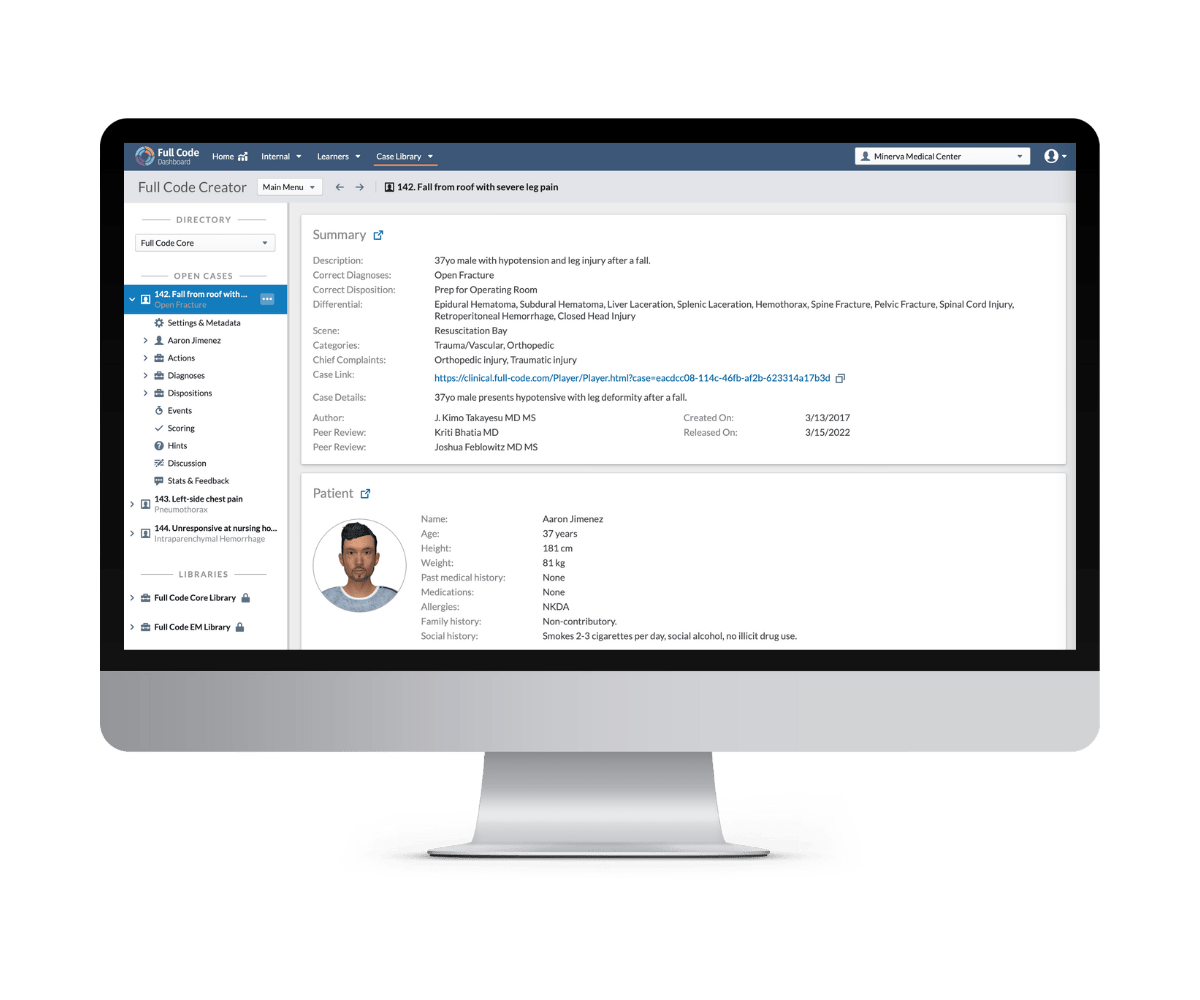
Full Code Creator
Customize Cases or Write Your Own
While Full Code offers 170+ pre-existing cases, the possibilities are endless with our custom case-authoring tool, Full Code Creator. Full Code Creator is a web-based authoring tool that makes scenario authoring easy with a library of template content.
Cross-Platform Implementation
Available on All Standard Devices*
Our Full Code Simulator can be used across mobile, tablet, or desktop devices.
*Certain older Android phones are not supported due to errors in their implementation of the 3D technologies used by Full Code.
More affordable medical simulation. Less hassle.
On-demand, realistic simulation training with virtual patients allows busy medical professionals to practice complex cases and improve their skills anytime, anywhere on the devices they already own, allowing for improved performance without additional in-person simulation training.



